Signed in as:
filler@godaddy.com
Signed in as:
filler@godaddy.com
What is plantar fasciitis?
The plantar fascia is a fibrous (thick strong connective tissue) band of tissue across the bottom of the foot. It connects the base of the toe area to the heel bone. Its’ function biomechanically is to assist the muscles in the foot. The plantar fascia also assist in re positioning (invert) the heel bone (calcaneous) upon push off in walking and running. Overall, this assists in re-supinating the foot from a pronated position. When it is over-strained, it inflames. Thus the “itis” (inflammation) and pain.
Shoes for Plantar Fasciitis
Although there is not one shoe that will help every plantar fasciitis patient, sometimes a simple treatment via the appropriate shoe for the type of foot one has may help resolve the problem. Do not fall for a simple “Shoes for plantar fasciitis” claim. It’s better to base the shoe upon your foot type. Typically look for shoes that have firmness around the heel bone (the counter of the shoe) and a rigid shank (does not bend in the middle of the shoe). Also, the inside of the shoe should have a cupped heel area and arch support. Arch support not only along the inside of the foot but also around the outside or lateral part of the foot as well as the front of the foot (by the ball, transverse arch).
Any excess tension or pull on the fascia can cause it to get micro-tears within the fascia. Excess tension can also cause the fascia to tear away from the heel bone. This can occur rather suddenly from an injury, such as landing hard on your foot. Also, this can be from chronic short term repetitive excess tension on the plantar fascia from faulthy biomechanics or foot/posture alignment. For example, if the foot is still pronated when it should be re supinating during the gait cycle, it can cause excess tension or pull on the fascia. As a result, tears and inflammation occur.
A classic symptom of plantar fasciitis is post static dyskinesia or pain after rest/non weight bearing. This occurs because the fascia is actually trying to heal itself. Inflammation is occuring, which is a normal healing response of the body. Patients will describe the pain as heel and arch pain, especially in the mornings. There are stages of healing and inflammation is the first stage. However, as typical, especially as we age, our bodies seem to over inflame.
Therefore, when no weight is on the foot, it inflames. Then when standing, the foot hurts because it is like stepping on a painful swollen area. The pain may diminish or even go away when walking. This is because the movement helps pump out the excess inflammation from the area. However, if the cause is from faulty biomechanics, walking will repeatedly re-damage the area and thus the cycle begins when the foot rests.
Treatment Options:
Treatment typically consists of two basics. First, reduce the inflammatory response. Second, address the cause of the fasciitis itself. Massage, compression, anti inflammatories, injections, and physical therapy may be helpful to minimize the painful inflammatory response.
Taping, strapping, muscle strengthening/physical therapy, cam boot immobilization and orthotics may help address the cause as well. Thus, allowing the area to thoroughly heal itself. In cases in which the fascia seems to not “Heal,” surgery or advanced injection therapy treatments like stem cell and growth hormone/plasma may be needed. ESWT (Shock Wave Therapy) has also been shown to be promising. However, like stem cell and growth hormone/plasma injections, it remains about 50-60% successful, depending on the study.
The latter treatments are typically reserved for long term resistant plantar fasciitis cases.
Plantar Fasciitis vs Plantar Fasciosis
Sometimes Plantar fasciitis is considered plantar fasciosis or vise versa. One is actually an inflammation and one is a degeneration of the fascia. Some will say after two weeks it is degenerating and thus can take longer to heal. I have found that even at two years of “Plantar Fasciitis,” we are able to obtain relief without surgery, injections nor the advanced therapy injections, etc.
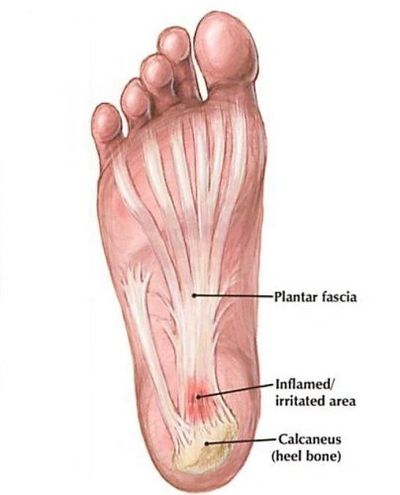
Example of where the plantar fascia is inflamed.
ArchMasters - Orthotics, Shoes & Footcare
101 Creekside Crossing, Suite 1500, Brentwood, TN 37027